As we age, we often focus on cardiovascular health or cognitive sharpness, but we frequently neglect the very foundation that keeps us upright: our feet. Senior foot health is not merely a matter of comfort; it is a critical component of survival and independence.
According to the Centers for Disease Control and Prevention (CDC), falls are the leading cause of fatal and non-fatal injuries among older adults. In fact, an older adult (age 65+) falls every second of every day. While factors like vision impairment or medication side effects play a role, poor foot health is a primary—and often preventable—culprit.
Understanding the connection between foot health and stability is the first step toward a safer, more active lifestyle. When feet are painful, stiff, or numb, the brain receives incomplete data about the ground, leading to hesitation and imbalance.
The Biomechanics of the Aging Foot
The human foot is a mechanical marvel consisting of 26 bones, 33 joints, and over 100 muscles, tendons, and ligaments. After decades of use, physiological changes are inevitable.
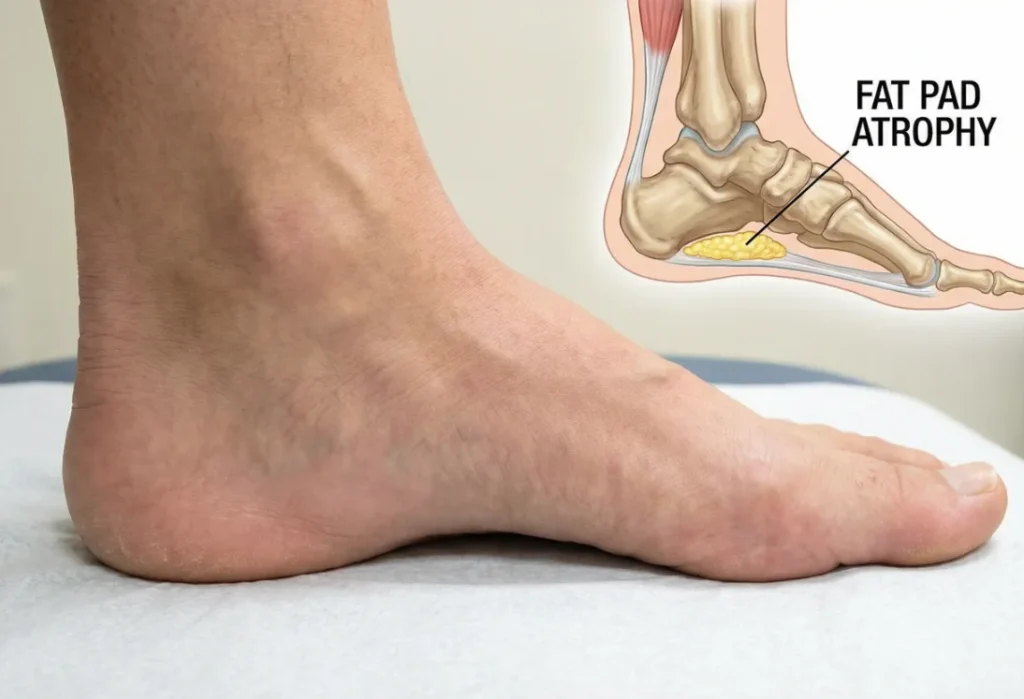
1. Fat Pad Atrophy
One of the most significant changes is the thinning of the plantar fat pads. These natural cushions under the heel and the ball of the foot act as shock absorbers. As collagen production decreases with age, these pads wear down—a condition known as fat pad atrophy. Walking on hard surfaces can become excruciating, causing seniors to alter their gait and compromise their balance.
2. Loss of Proprioception
Proprioception is the body’s ability to sense its position in space. As nerve function naturally diminishes, this “positional sense” fades. A senior may believe they have lifted their foot high enough to clear a rug when they haven’t, leading to trips.
3. Reduced Joint Flexibility
Connective tissues lose elasticity over time, leading to stiffness in the ankles and toes. If the ankle cannot flex properly (dorsiflexion), the toes are more likely to catch on uneven surfaces.
4. Spreading and Flattening
Over time, ligaments can stretch, causing the foot to flatten and widen. Wearing shoes that are now too narrow compresses the foot, causing pain and reducing the stable surface area available for balance.
Common Conditions That Increase Fall Risk
Pain is a powerful driver of behavior. When feet hurt, we subconsciously change how we move. These compensatory movements are major barriers to stability.
- Bunions (Hallux Valgus): This bony bump at the base of the big toe alters weight-bearing ability. Since the big toe is crucial for “push-off,” misalignment causes a loss of propulsion and stability.
- Corns and Calluses: Thickened, hardened layers of skin caused by repeated friction and pressure. These can feel like walking on pebbles. To avoid pressure, seniors may shift their weight to the outside of the foot, creating a precarious base.
- Onychomycosis (Fungal Nails): Thick, distorted nails can press against shoes, causing sharp pain and reducing the sensory feedback the toes receive from their environment.
- Edema (Swelling): Common in those with circulation issues, swelling can make shoes fit poorly, forcing seniors to wear loose slippers or go barefoot—both of which significantly increase fall risk.
The Diabetes Connection
For those managing diabetes, foot care is a matter of limb preservation and safety. High blood sugar levels can lead to:
- Diabetic Neuropathy: Nerve damage that results in a loss of sensation. If a senior cannot feel the ground, they rely entirely on vision for balance. In low-light conditions, the risk of a fall skyrockets.
- Peripheral Arterial Disease (PAD): Poor circulation slows the healing of cuts or blisters. An open wound changes how a person walks to avoid pain, leading to gait irregularities.
Resource: Learn more about our specializedDiabetic Foot Care and Managementservices.
The Role of Custom Orthotics
For many seniors, off-the-shelf footwear doesn’t provide enough support. Custom orthotics are a powerful tool for restoring stability and confidence.
- Realigning the Skeleton: Orthotics can correct over-pronation (rolling inward) or supination (rolling outward), creating a neutral skeletal structure that reduces strain on the knees and hips.
- Replacing Lost Cushioning: For those with fat pad atrophy, we design orthotics with specialized materials like Plastazote or Poron to mimic natural shock absorption.
- Offloading Pressure: For seniors with diabetes or painful calluses, custom orthotics can be designed with “cut-outs” to float painful areas, allowing for a normal, stable gait.
Choosing Shoes for Stability
The right footwear is your first line of defense. Many seniors prefer slip-on shoes or soft slippers, but these are often the most dangerous options.
The “Safe Shoe” Checklist:
- Firm Heel Counter: The back of the shoe should be stiff to lock the heel in place and prevent ankle rolling.
- Low, Wide Heel: A slight elevation (less than 1 inch) with a wide base offers the best stability.
- Non-Slip Soles: Look for rubber soles with moderate tread. Avoid heavy lug soles that can catch on carpet.
- Adjustable Fastenings: Velcro closures are excellent for those with arthritis, ensuring the shoe stays secure without the struggle of laces.
Proactive Prevention Exercises For Senior Foot Health
Maintaining foot strength is essential for “clearing” the ground while walking. We recommend consulting a professional, but these daily movements can help:
- Ankle Pumps: While sitting, point your toes down and then pull them up toward your shin to improve circulation.
- Toe Taps: Keep your heels down and tap your toes rapidly to strengthen the shin muscles.
- The “Stork” Stand: Practice balancing on one foot while holding onto a sturdy counter to improve proprioception.
- Towel Scrunches: Use your toes to pull a small towel toward you to strengthen the arch muscles.
Senior Foot Health Conclusion: A Step Toward Independence
Falls are not an inevitable consequence of aging. They are often the result of untreated issues that accumulate over time. By prioritizing senior foot health—treating pain, wearing proper orthopedic footwear, and using custom orthotics—seniors can build a solid foundation for the years ahead.
When your feet are stable, your confidence grows. And when a senior is confident in their step, they remain active, social, and independent.
Is foot pain affecting your balance? Book an Orthopedic Assessment with our team today to find the right solution for your mobility.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. For more information on senior health in Canada, visit Health Canada.





