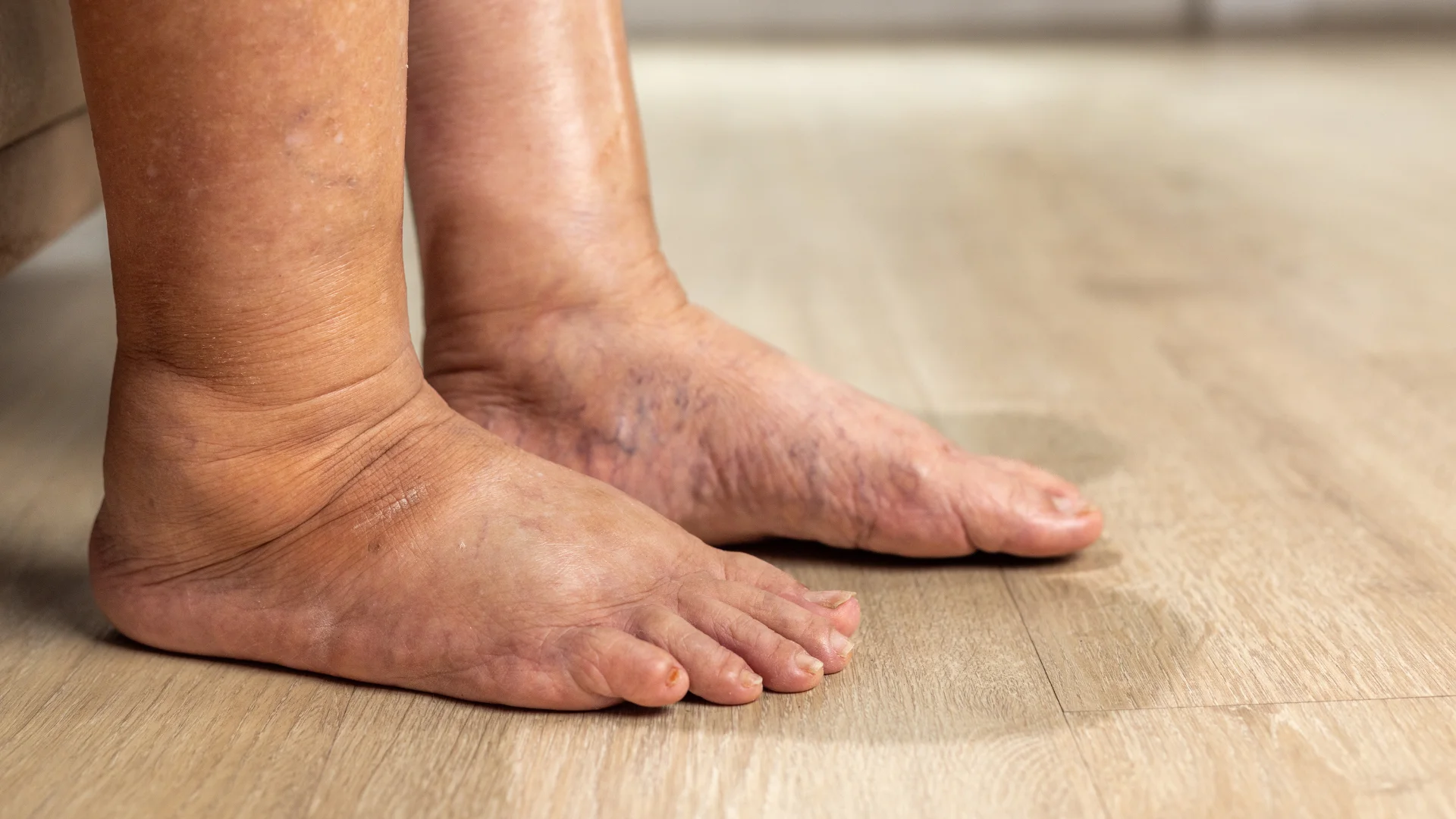
Living with diabetes requires a daily balancing act. Between monitoring blood glucose levels, managing your diet, and staying active, it is easy to overlook the parts of your body that are furthest away from your eyes: your feet.
However, in the medical and orthotic communities, diabetic foot care is never treated as an afterthought. It is a critical, life-saving daily practice. For someone living with diabetes, a minor foot issue—like a small blister from a tight shoe or a pebble inside a boot—can rapidly escalate from a mild annoyance into a severe medical emergency.
At Custom Orthopedic & The Walk Shoppe in Edmonton, we work closely with diabetic patients to preserve their mobility and protect their limbs. Whether you are newly diagnosed or have been managing your condition for decades, this guide will explain exactly why protective footwear and custom orthotics are non-negotiable components of your overall health plan.
1. The Diabetes-Foot Connection: Understanding the Risks
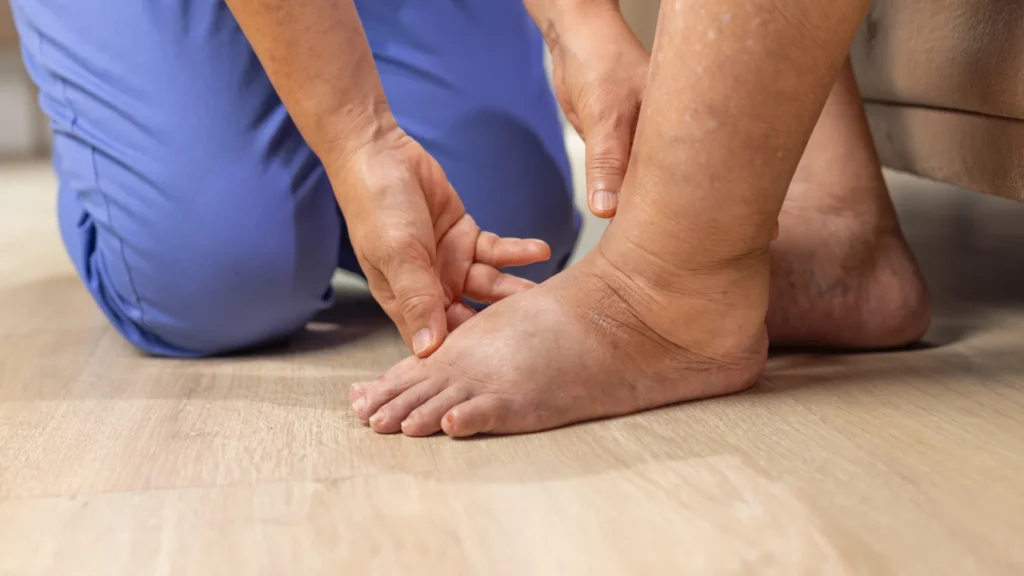
To understand why diabetic foot care is so urgent, you have to understand how diabetes physically alters your lower extremities. The disease primarily attacks the feet through two distinct, dangerous pathways:
Peripheral Neuropathy (Loss of Sensation)
Over time, elevated blood sugar levels damage the delicate nerve fibers in your legs and feet. This condition, known as diabetic peripheral neuropathy, causes a gradual loss of sensation. You might experience tingling, burning, or—most dangerously—complete numbness.
If a person without diabetes steps on a sharp object or wears a shoe that rubs against their heel, pain signals their brain to stop, take off the shoe, and fix the problem. A person with severe neuropathy does not receive that pain signal. They might walk on a bleeding blister or a fractured bone all day without ever feeling it. By understanding what your feet are telling you, or in this case, what they aren’t telling you, you can recognize the urgency of visual inspections.
Poor Circulation (Peripheral Arterial Disease)
Diabetes also damages blood vessels, decreasing the flow of oxygen-rich blood to the feet. When circulation is compromised, your body’s natural healing process slows down to a crawl. A minor scrape that would take a healthy person three days to heal might take a diabetic patient three months.
When you combine neuropathy (failing to notice an injury) with poor circulation (the inability to heal that injury), you create the perfect storm for diabetic foot ulcers, deep infections, and ultimately, amputations.
2. Protective Footwear: Your First Line of Defense
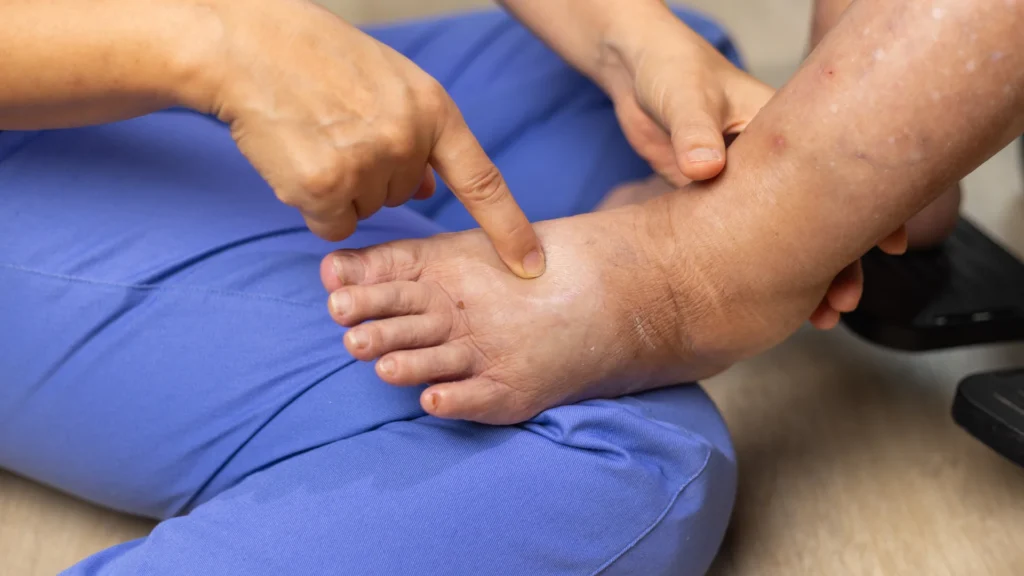
Because your feet cannot be trusted to feel pain, your shoes must act as a protective armor. Regular, off-the-shelf footwear from a standard shoe store is often designed for fashion over function, featuring narrow toe boxes, hard internal seams, and stiff materials. For a diabetic, these features are dangerous.
True diabetic footwear is engineered differently. Here is what to look for when selecting shoes for proper diabetic foot care:
- Extra Depth: Diabetic shoes are built with extra depth to accommodate swollen feet (edema) and thick, custom-molded orthotics without crushing the top of the foot against the shoe. If you struggle with swelling, explore these key steps to treat edema.
- Wide, High Toe Box: Your toes need room to wiggle. A restrictive toe box causes toes to overlap, leading to friction and ulcers on the joints.
- Seamless Interiors: Run your hand inside the shoe. A proper diabetic shoe has a smooth, seamless lining. A single raised seam can rub against a neuropathic foot and cause a wound within hours.
- Firm Heel Counters & Rocker Soles: A firm heel counter provides stability, while a rigid rocker sole reduces the pressure placed on the ball of the foot during the push-off phase of walking.
3. Custom Orthotics: Essential Off-Loading and Pressure Relief
While protective shoes provide the outer shell, custom orthotics provide the internal biomechanical foundation.
When you walk, certain areas of your foot—typically the heel and the metatarsal heads (the ball of the foot)—bear the brunt of your body weight. If you have a foot deformity or altered gait, this pressure becomes highly localized. High pressure leads to the rapid buildup of thick skin. While managing this is important (see our practical steps to combat callus formation), in a diabetic foot, a thick callus can actually act like a rock inside the shoe, pressing inward and breaking down the healthy tissue beneath it until an ulcer forms.
Custom orthotics designed for diabetic foot care serve a specific medical purpose called off-loading.
How Diabetic Orthotics Work
Unlike the rigid plastic orthotics given to athletes to correct severe overpronation, diabetic orthotics are typically made from specialized, multi-density foams (like Plastazote).
- Total Contact: The orthotic is molded to match the exact, unique contours of your foot. This ensures your weight is distributed evenly across the entire surface area of the foot, rather than focused on one or two high-pressure hot spots.
- Shock Absorption: The top layer is designed to compress and shear with the foot, reducing the friction that causes blisters and calluses.
- Accommodation: If you already have a vulnerable area or an active, healing ulcer, the orthotist can create a “relief” or a depression in the orthotic to completely float that specific area, ensuring zero pressure touches it while you walk.
Understanding how your custom orthotics are made can help you appreciate the precision required to protect vulnerable, neuropathic feet.
4. The Threat of Charcot Foot
One of the most severe complications of diabetic neuropathy is Charcot (pronounced shar-ko) foot. Because of the lack of sensation and compromised bone density, a diabetic patient may experience micro-fractures in the bones of the foot. Without pain to stop them, they continue walking on these broken bones.
Eventually, the joints collapse, and the arch of the foot completely drops, creating a “rocker-bottom” deformity. This new, unnatural shape makes the foot incredibly susceptible to ulcers. If you notice sudden swelling, redness, and heat in your foot, even without pain, seek immediate medical attention. We have a dedicated guide on the essential steps to manage Charcot foot effectively using specialized bracing and custom orthotics.
5. Daily Diabetic Foot Care: A Step-by-Step Routine
Relying on great footwear and orthotics is only half the battle. Excellent diabetic foot care requires strict, daily vigilance. Incorporate this routine into your life every single day:
- The Daily Inspection: Look at the top, bottom, and sides of your feet, as well as between your toes. Look for redness, cuts, blisters, cracks, or any change in skin color. If you cannot see the bottom of your feet, use a hand mirror or ask a family member for help.
- Wash, Don’t Soak: Wash your feet daily with warm (not hot!) water and mild soap. Never soak your feet, as this breaks down the skin and makes it vulnerable to tearing. Because of neuropathy, always test the water temperature with your elbow or a thermometer before stepping in.
- Dry Thoroughly: Pat your feet dry with a soft towel. Be meticulous about drying the spaces between your toes, as trapped moisture can lead to fungal infections.
- Moisturize Carefully: Apply a good quality moisturizer to the tops and bottoms of your feet to prevent dry, cracking skin. Never put lotion between your toes.
- Never Walk Barefoot: Not in your house, not at the beach, and not at the public pool. A stray tack on the carpet or a hot piece of pavement can cause severe damage. Always wear supportive, protective footwear.
- Inspect Your Shoes Before Wearing: Before putting your shoes on, run your hand around the inside. Check for pebbles, torn linings, or anything that could cause friction.
External Resource: For comprehensive information on managing your blood glucose and overall health, we highly recommend reviewing the resources provided by Diabetes Canada.
6. The Edmonton Winter Challenge
Managing diabetes in Alberta comes with its own unique set of challenges. Our brutal winters mean navigating snow, ice, and freezing temperatures.
Cold weather causes blood vessels to constrict, further reducing circulation to your extremities. Furthermore, heavy, poorly-fitting winter boots can cause friction, while thick winter socks can make a normally well-fitting shoe dangerously tight.
It is vital that your winter footwear accommodates your diabetic orthotics without compressing your foot. When preparing for the season, be sure to read our guide on how to choose orthotic-friendly boots and prevent cold-weather foot pain to ensure you stay warm, stable, and ulcer-free from November to March.
Your Feet Are Irreplaceable. Protect Them
When you are living with diabetes, diabetic foot care is not a luxury; it is the foundation of your independence. Prevention is infinitely easier—and far less costly to your quality of life—than treating a severe complication after it has already occurred. By combining daily visual inspections with professional, appropriately fitted footwear and pressure-relieving custom orthotics, you can keep your feet healthy and stay active for years to come.
Are your current shoes feeling tight, or are you concerned about high-pressure areas on your feet? Would you like me to help you set up an appointment for a diabetic foot assessment and orthotic fitting?